Find out everything you need to know about Plantar Fasciitis
As we get older, getting out of bed in the morning can be a daunting task. Especially if you’re a lifter. Some of us can’t straighten up. We slide off and then slump over the bed, allowing for what appears to be a moment of prayer but it’s actually a chance to relish the last vestiges of a gravity-free day. As we accordion-walk our way to the bathroom, various aches, pains and mental issues creep in. Growing older as a weightlifter is a great way to stay humble, if you’re concerned about spiritual growth that is. For others… it’s just a pain in the gluteus.
Even with 45 minutes of cardio a day, stretching, powerlifting, weight training and personal training… at age 55 it’s getting harder for me to get out of bed.
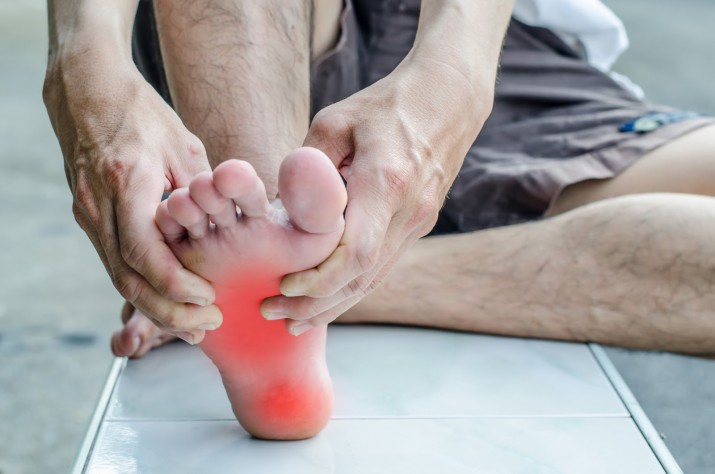
But not nearly as hard as for those who suffer from Plantar Fasciitis. If the bottom of your heels hurt after sleeping, sitting or during exercise, you may have PF. There’s a fibrous “rubber band” that stretches along the bottom of your foot. It’s supposed to be nice and springy, absorbing the stress and pressures you place on your feet. But too much stress without adequate flexibility will cause injury to the tissue. As we age, we lose elasticity, plasticity and lubrication… affecting us in places like the Plantar Fascia and Achilles tendon. The body responds with painful inflammation and hence you’re tip-toing to the bathroom. The pain is sharp, severe enough to discourage anyone from doing physical activity.
It may feel like a bone spur, but it may not be a spur. And good news here: if you do have a spur, it is probably NOT the cause of your pain. Again, heel spurs do not cause much foot pain (This from the American Academy of Orthopedic Surgeons). Only one out of ten people have heel spurs, but only 5% of those have foot pain. So it’s important to note that spurs do not cause plantar fasciitis, and therefore your pain can be treated without removing the spur.
If your doctor wants to take X-rays, please don’t treat him/her like he/she’s the devil. It’s common for doctors to use X-rays to rule out arthritis or hairline fractures. Typically an MRI will be suggested only when initial treatments don’t relieve pain. Surgery is almost never considered without at least 12 months of non-surgical treatment. Most PF sufferers do well after surgery. But surgery can also result in more chronic pain and immobility. Complications of PF surgery include failure to relieve pain and nerve damage. For this reason, The American Academy of Orthopedic Surgeons recommends surgery only after all nonsurgical measures have been exhausted. So let’s avoid it altogether if possible, okay?
Treating and/or avoiding Plantar Fasciitis
If you’re overweight, have high arches, are engaged in repetitive exercise and/or have begun a new activity, then you’ll want to nip PF in the bud before it stops you from doing the things you love. Here are the things you can do to be proactive in avowing and treating PF:
- Stretches – Plantar fasciitis is awakened by taut muscles in your feet and calves. Stretching and massaging your calves, plantar fascia, feet and Achilles tendon is the most effective way to relieve the pain and avoid this condition. I always guide my clients into stretching after a workout. Some of them complain that my flexibility lessons are a waste of their time and money. I tell them it’s not about the money. It’s my way or the highway on this subject.
- Cortisone injections – Cortisone is an anti-inflammatory steroid, injected into the plantar fascia to reduce inflammation and pain. Your doctor may limit injections, and rightly so. Too many steroid shots can cause ruptures which lead to “flat foot” and exacerbated pain.
- Supportive shoes and orthotics – Get supportive shoes with thick soles and cushioning to reduce pain. Please don’t cling onto those dilapidated, stained, lopsided shoes for one more second. Spend some bucks and spring for a GOOD pair. A cushioned shoe reduces tension and micro-trauma to the Plantar Fascia. Soft silicone heel pads, store-bought and custom orthotics may also prove helpful.
- Night splints – Most folks sleep with their feet pointed down, which relaxes the plantar fascia and causes morning heel pain. Try sleeping with the PF stretched instead. I do this with my toes up against my blanket. If you can’t do it, ask your doctor about a night splint. A Night splint is not for wimps. It is uncomfortable but very effective. Once the pain is gone, you won’t need to wear it anymore.
- Physical therapy – A personal trainer can show you how to stretch, but if you can’t do it yourself, a Physical Therapist will stretch your muscles and fascia for you. Physical Therapists are also licensed to apply specialized ice treatments, massage, and medication to decrease inflammation.
- Extracorporeal shockwave therapy (ESWT) – Powerful shockwaves that stimulate the healing process in damaged tissue. This is a fairly new procedure. Two of my friends have had this done with terrific results, but clinically it is still not a tried and true procedure. Because of the minimal risk involved, ESWT is sometimes preferred before surgery is considered.



